Der Darmbakterientest, der Ihnen einen Einblick in Ihre Gesundheit gibt
- Mikrobiom -Testkit
- 16S -Analyse
- Wissenschaftliche Erkenntnisse
Erfahren Sie mehr über
die Mikrobiota
Last updated: 5-5-2026
Stomach pain after a healthy salad, bloating without a clear cause, or bowel movements that are different every day. If you have Irritable Bowel Syndrome (IBS), this sounds painfully familiar. You have probably already tried some diets and supplements, but the advice often contradicts itself.
More and more scientific research points to an important player in the field: your microbiome. In this blog, you can read about the role your microbiome plays in IBS and how that insight can help reduce your symptoms.
IBS is a chronic condition that is very common: around five to ten percent of the Dutch population is affected by it. In IBS, the intestines are hypersensitive and respond to the smallest trigger. The result: stomach pain, bloating, flatulence, bowel movements that go in every direction, and so on. These symptoms not only differ from person to person, but can also be completely different from one day to the next in the same person.
The exact cause is not yet fully known. Scientists are actively looking for answers: what causes IBS, and how can the symptoms be reduced, or even resolved completely? In doing so, they mainly look at four major factors: stress, exercise, nutrition and the microbiome.
Please note!
Blood in the stool, fever and sudden, unexplained weight loss are not symptoms of IBS. If you experience these symptoms, contact your GP immediately.
Are you 50 years or older and are you suddenly experiencing symptoms that fit with IBS? Then contact your GP as well. Another condition or disease may be involved. The risk of serious intestinal disorders increases with age.
In these cases, it is not a good time to do a microbiome test, because your microbiome is probably different from how it normally looks.
And that microbiome is a world of its own. It consists of billions of bacteria, yeasts and other microbes that live in your intestines. More and more research shows that the composition of the microbiome in people with IBS is different from that of people without daily intestinal complaints. And that difference can tell us a lot about why your intestines sometimes react so strongly.
Think of your microbiome as an ecosystem: a rainforest full of different species, each with its own task. Some bacteria help break down your food, others make vitamins or protect you against intruders. In people with IBS, that rainforest often appears to be less diverse: certain beneficial species are in the minority, while other bacteria become dominant. This can lead to more gas formation, a sensitive intestinal wall and sometimes even mild inflammatory reactions. The difficult part is: exactly which bacteria are out of balance differs per person. That is why there is no one-size-fits-all solution. What works for one person may do nothing for another, or may even worsen symptoms. That is exactly why we are increasingly looking at personal microbiome analyses as the path toward more targeted advice.
Researchers are discovering more and more about the link between IBS and the microbiome. These are the most important insights so far:
Because IBS and the microbiome are slightly different for everyone, it is difficult to truly get your symptoms under control based on general advice. You can endlessly experiment with nutrition, supplements and lifestyle, but without knowing exactly what is happening in your intestines, it remains a shot in the dark.
A microbiome analysis does provide that personal picture: which bacteria are abundantly present in you, which are actually missing and how that may be related to your symptoms.
The results of the test give you a clear picture of who is ‘living’ in your intestines, and help you make more targeted adjustments to your nutrition or lifestyle. You do not receive a standard list of tips, but advice that fits your unique microbiome. This can help you answer for yourself which nutrition and lifestyle choices are the right ones for you.
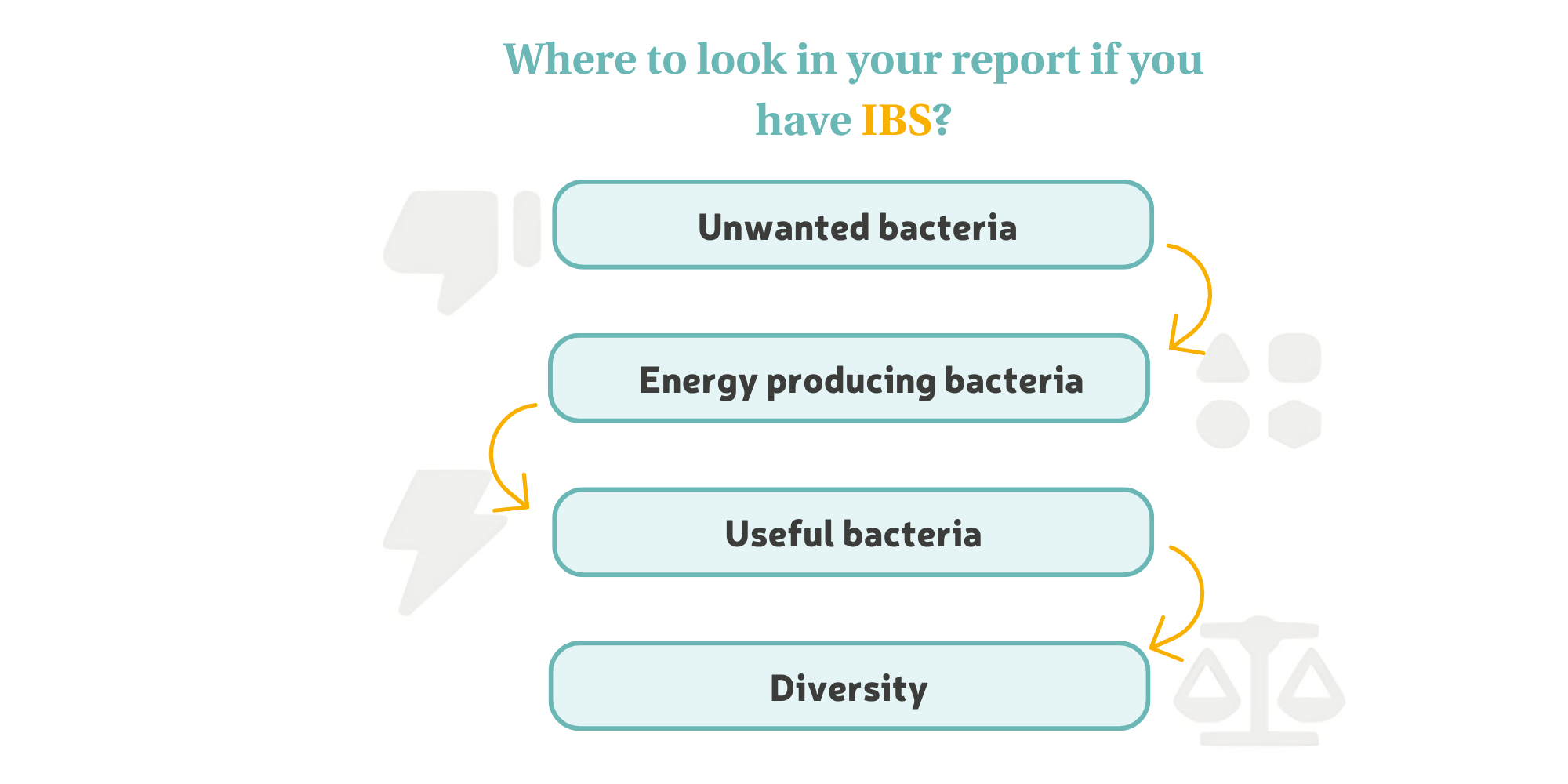
After doing a microbiome test, you receive a report that explains your gut health step by step in four chapters. The order is based on what is usually most important. Do you have IBS? Then it is better to follow an adjusted order, because in IBS other bacterial groups often have more influence on your symptoms. Download here the guide to reading your microbiome report if you have IBS.
IBS is a complex puzzle in which nutrition, stress, exercise and your microbiome are all pieces. Science is showing more and more clearly that this bacterial community in your intestines is extremely important. And partly because no two people, nor microbiomes, are the same, there is no one-size-fits-all solution. Doing a microbiome test could therefore help you by giving you insight into which adjustments you specifically could make in your life to potentially reduce your symptoms.
Discover here how our test works exactly, or compare our test here with other methods.
Do you have IBS, but have not yet managed to get rid of the symptoms? MyMicroZoo is looking for people with IBS symptoms who are willing to follow the low FODMAP diet, and in doing so learn more about their microbiome. You may do a microbiome test with us free of charge. Read more information about the study on this page.
References:
Carroll, I. M., Ringel-Kulka, T., Siddle, J. P., & Ringel, Y. (2012). Alterations in composition and diversity of the intestinal microbiota in patients with diarrhea-predominant irritable bowel syndrome. Neurogastroenterology and motility, 24(6), 521–e248. https://doi.org/10.1111/j.1365-2982.2012.01891.x
Chassard, C., Dapoigny, M., Scott, K. P., Crouzet, L., Del'homme, C., Marquet, P., Martin, J. C., Pickering, G., Ardid, D., Eschalier, A., Dubray, C., Flint, H. J., & Bernalier-Donadille, A. (2012). Functional dysbiosis within the gut microbiota of patients with constipated-irritable bowel syndrome. Alimentary pharmacology & therapeutics, 35(7), 828–838. https://doi.org/10.1111/j.1365-2036.2012.05007.x
Jeffery, I. B., O'Toole, P. W., Öhman, L., Claesson, M. J., Deane, J., Quigley, E. M., & Simrén, M. (2012). An irritable bowel syndrome subtype defined by species-specific alterations in faecal microbiota. Gut, 61(7), 997–1006. https://doi.org/10.1136/gutjnl-2011-301501
Kushkevych, I., Leščanová, O., Dordević, D., Jančíková, S., Hošek, J., Vítězová, M., Buňková, L., & Drago, L. (2019). The Sulfate-Reducing Microbial Communities and Meta-Analysis of Their Occurrence during Diseases of Small–Large Intestine Axis. Journal of Clinical Medicine, 8(10), 1656. https://doi.org/10.3390/jcm8101656
Labus, J. S., Hollister, E. B., Jacobs, J., Kirbach, K., Oezguen, N., Gupta, A., Acosta, J., Luna, R. A., Aagaard, K., Versalovic, J., Savidge, T., Hsiao, E., Tillisch, K., & Mayer, E. A. (2017). Differences in gut microbial composition correlate with regional brain volumes in irritable bowel syndrome. Microbiome, 5(1), 49. https://doi.org/10.1186/s40168-017-0260-z
Liu, H. N., Wu, H., Chen, Y. Z., Chen, Y. J., Shen, X. Z., & Liu, T. T. (2017). Altered molecular signature of intestinal microbiota in irritable bowel syndrome patients compared with healthy controls: A systematic review and meta-analysis. Digestive and liver disease : official journal of the Italian Society of Gastroenterology and the Italian Association for the Study of the Liver, 49(4), 331–337. https://doi.org/10.1016/j.dld.2017.01.142
Liu, Y., Li, W., Yang, H., Zhang, X., Wang, W., Jia, S., Xiang, B., Wang, Y., Miao, L., Zhang, H., Wang, L., Wang, Y., Song, J., Sun, Y., Chai, L., & Tian, X. (2021). Leveraging 16S rRNA Microbiome Sequencing Data to Identify Bacterial Signatures for Irritable Bowel Syndrome.
Malinen, E., Rinttilä, T., Kajander, K., Mättö, J., Kassinen, A., Krogius, L., Saarela, M., Korpela, R., & Palva, A. (2005). Analysis of the fecal microbiota of irritable bowel syndrome patients and healthy controls with real-time PCR. The American journal of gastroenterology, 100(2), 373–382. https://doi.org/10.1111/j.1572-0241.2005.40312.x
Nagel, R., Traub, R. J., Allcock, R. J., Kwan, M. M., & Bielefeldt-Ohmann, H. (2016). Comparison of faecal microbiota in Blastocystis-positive and Blastocystis-negative irritable bowel syndrome patients. Microbiome, 4(1), 47. https://doi.org/10.1186/s40168-016-0191-0
Pittayanon, R., Lau, J. T., Yuan, Y., Leontiadis, G. I., Tse, F., Surette, M., & Moayyedi, P. (2019). Gut Microbiota in Patients With Irritable Bowel Syndrome-A Systematic Review. Gastroenterology, 157(1), 97–108. https://doi.org/10.1053/j.gastro.2019.03.049
Prikkelbare Darm Syndroom Belangenorganisatie. (2022, November 29). Diagnose - prikkelbare darm syndroom Belangenorganisatie. https://www.pdsb.nl/diagnose/
Rajilić-Stojanović, M., Biagi, E., Heilig, H. G., Kajander, K., Kekkonen, R. A., Tims, S., & de Vos, W. M. (2011). Global and deep molecular analysis of microbiota signatures in fecal samples from patients with irritable bowel syndrome. Gastroenterology, 141(5), 1792–1801. https://doi.org/10.1053/j.gastro.2011.07.043
Rangel, I., Sundin, J., Fuentes, S., Repsilber, D., de Vos, W. M., & Brummer, R. J. (2015). The relationship between faecal-associated and mucosal-associated microbiota in irritable bowel syndrome patients and healthy subjects. Alimentary pharmacology & therapeutics, 42(10), 1211–1221. https://doi.org/10.1111/apt.13399
Salminen, S., von Wright, A., Morelli, L., Marteau, P., Brassart, D., de Vos, W. M., Fondén, R., Saxelin, M., Collins, K., Mogensen, G., Birkeland, S. E., & Mattila-Sandholm, T. (1998). Demonstration of safety of probiotics -- a review. International journal of food microbiology, 44(1-2), 93–106. https://doi.org/10.1016/s0168-1605(98)00128-7
Sheikh Sajjadieh, M. R., Kuznetsova, L. V., & Bojenko, V. B. (2012). Dysbiosis in ukrainian children with irritable bowel syndrome affected by natural radiation. Iranian journal of pediatrics, 22(3), 364–368.
Su, Q., Tun, H. M., Liu, Q., Yeoh, Y. K., Mak, J. W. Y., Chan, F. K., & Ng, S. C. (2023). Gut microbiome signatures reflect different subtypes of irritable bowel syndrome. Gut Microbes, 15(1), 2157697. doi: https://doi.org10.1080/19490976.2022.2157697
Vich Vila, A., Imhann, F., Collij, V., Jankipersadsing, S. A., Gurry, T., Mujagic, Z., Kurilshikov, A., Bonder, M. J., Jiang, X., Tigchelaar, E. F., Dekens, J., Peters, V., Voskuil, M. D., Visschedijk, M. C., van Dullemen, H. M., Keszthelyi, D., Swertz, M. A., Franke, L., Alberts, R., Festen, E. A. M., … Weersma, R. K. (2018). Gut microbiota composition and functional changes in inflammatory bowel disease and irritable bowel syndrome. Science translational medicine, 10(472), eaap8914. https://doi.org/10.1126/scitranslmed.aap8914
Wang, L., Alammar, N., Singh, R., Nanavati, J., Song, Y., Chaudhary, R., & Mullin, G. E. (2020). Gut Microbial Dysbiosis in the Irritable Bowel Syndrome: A Systematic Review and Meta-Analysis of Case-Control Studies. Journal of the Academy of Nutrition and Dietetics, 120(4), 565–586. https://doi.org/10.1016/j.jand.2019.05.015
Zeber-Lubecka, N., Kulecka, M., Ambrozkiewicz, F., Paziewska, A., Goryca, K., Karczmarski, J., Rubel, T., Wojtowicz, W., Mlynarz, P., Marczak, L., Tomecki, R., Mikula, M., & Ostrowski, J. (2016). Limited prolonged effects of rifaximin treatment on irritable bowel syndrome-related differences in the fecal microbiome and metabolome. Gut microbes, 7(5), 397–413. https://doi.org/10.1080/19490976.2016.1215805
Zhong, W., Lu, X., Shi, H., Zhao, G., Song, Y., Wang, Y., Zhang, J., Jin, Y., & Wang, S. (2019). Distinct Microbial Populations Exist in the Mucosa-associated Microbiota of Diarrhea Predominant Irritable Bowel Syndrome and Ulcerative Colitis. Journal of clinical gastroenterology, 53(9), 660–672. https://doi.org/10.1097/MCG.0000000000000961
KvK nummer: 65867637
Website door: Ratio Design
Diese Website verwendet essentielle Cookies, um die korrekte Funktionalität zu gewährleisten. Um unsere Website zu verbessern, können wir auch optionale Cookies verwenden.
Mehr Informationen